Taking care of your bladder and bowels: An expert’s top tips
2 April 2019
Please note, Back Up are not medical professionals. We are just sharing information from a healthcare professional experienced in their field. Make sure that you contact your GP or spinal centre if you are concerned about your bladder or bowels.
No matter your level of injury, taking care of your bladder and bowels is important. That’s why we spoke to Advanced Nurse Practitioner Tracey Geddis about her top tips for managing your bladder and bowels.
How do you prevent urinary tract infections (UTI)?
At the moment, the only solution for controlling and suppressing chronic UTIs is long-term antibiotics. However, you can take steps to prevent UTIs from developing:
• Increase your fluid intake – Two to three litres per day is recommended.
• Waterfall D-mannose – This is a type of sugar, but unlike sucrose or fructose, it does not interfere with blood sugar regulation or metabolism. Research also concluded that D-mannose had a significant effect in reducing the risk of a recurrent UTI, similar to that of prescription medication.
• Vitamin C – The research on vitamin C for UTI prevention is still in its early stages. There is some evidence to suggest vitamin C may be an effective remedy for urinary tract infections involving nitrate-reducing bacteria. Vitamin C as a supplement is generally safe, but certain medical conditions and mega doses should first be discussed with your doctor.
• Avoid constipation – Constipation can increase the chances of bladder infections in two ways. First, if stool gets stuck in the rectum, it inhibits the emptying of the bladder, which can cause some people to retain urine. Urine retention leads to stagnant urine, which will lead to a bladder infection. The loaded rectum can also press on the bladder and preventing an indwelling catheter from draining properly.
• Regular check-ups with your spinal unit – This is a chance to discuss any problems you are having with your bladder and/or bowels and ask for any further advice to prevent infection.
• Bladder management – Your bladder must be emptied regularly and completely to prevent infection. If you are having recurring infections, ensure you are emptying completely.
• Sex – Spermicides and barrier contraceptives can sometimes cause a UTI. Not all condoms increase your chances to contract a UTI, so the trick is to look for condoms without spermicide.
• Age – After menopause, our bodies produce less oestrogen. Oestrogen helps maintain the strength and thickness of the vaginal wall and the urethral lining and encourages vaginal lubrication. Studies demonstrate that oestrogen treatment delivered vaginally may help prevent repeat urinary tract infections.

Keep hydrated – Drinking two to three litres of water a day is essential for healthy bladder and bowels[/caption]
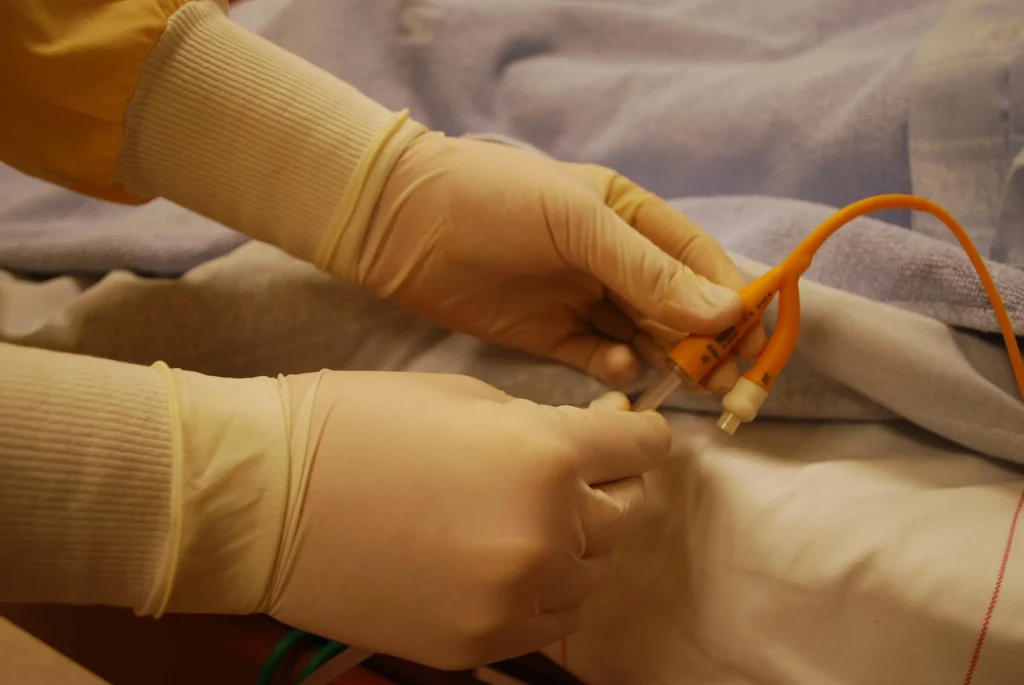
Best practice for catheter use
• For indwelling catheters (urethral and/or supra pubic catheters), regular catheter changes are required. Indwelling long term catheters are licensed for three months, however, in some spinal units we recommend they are changed every four to six weeks to prevent blockages.
• Anchorage of catheters is recommended with securement devices like StatLock or Clinifix. There are also silicone options for people with sensitive skin like the Shop Optimum Multi Fix Gentle. These prevent the catheter kinking, being pulled during transfers, or being trapped in the groin.
• Catheter valves (Flip flo valves) come in different forms, so it’s good to research what kind will suit you best – Especially for patients with limited hand dexterity, as cable ties can be added to aid opening and closure.
• Guidelines and research advise that you change your leg bag every five to seven days, and attach a two litre night bag when you go to bed. This reduces infection risk.
• Always keep hydrated. Normally two to three litres of fluid daily will keep urine clear.
• Always practice good general hygiene around a catheter site.

What diet changes can make bowel management easier?
Maintaining a formed stool consistency (neither too hard nor too loose) helps to maintain a successful bowel programme and prevent constipation. These are some steps you can take to keep up a balanced diet:
• Eat at least five portions of a variety of fruits and vegetables every day.
• Base meals on potatoes, bread, rice, pasta or other starchy carbohydrates – choosing wholegrain versions where possible.
• You can have some dairy or dairy alternatives (such as soya drinks), but try to choose low fat and low sugar options.
• Eat some beans, pulses, fish, eggs, meat and other proteins (including two portions of fish every week, one of which should be oily).
• Choose unsaturated oils and spreads and eat in small amounts.
• If consuming foods and drinks high in fat, salt or sugar, aim to have these less often and in small amounts.
• Increasing dietary fibre can encourage transit time and form a bulkier stool that will pass easier. Be sure to drink plenty of fluids if you increase the fibre in your diet to prevent constipation.
Types of fibre
Insoluble fibre – found in fruit skins, fibrous vegetables e.g. carrots, wholemeal/wholegrain flour, breads, bran and cereals. Insoluble fibre passes through the digestive system intact. It helps you to pass waste more easily by making the stools soft and bulky. This helps to prevent constipation.
Soluble fibre – found in oats, rye, beans, peas, lentils and other fruit and vegetable flesh. Soluble fibre forms a gel when mixed with liquid and increases the time taken for the stomach to empty. This means that glucose is released and absorbed slowly, which helps to regulate blood glucose levels. Soluble fibre also binds to excess cholesterol in the digestive system and prevents it from being absorbed. This helps to lower bad cholesterol in the blood.
While oats and other cereals are a good source of fibre, some cereal products such as flapjacks, biscuits and cereal bars can contain large amounts of saturated fat and sugar. Check food labels to help you make healthy choices.
If you have hard stools:
• Increase fluid intake
• Have at least five portions of fruits and vegetables per day
• Gradually increase insoluble fibre
• If intake of insoluble fibre is very high, try reducing the insoluble fibre gradually
• If changes to fibre content of diet makes no difference, return to normal balanced diet.
• Consider stool softener (laxative)
If you have loose stools:
Reduce stimulant foods (foods that over stimulate bowel activity or draw excessive fluid into the colon) such as…
• Alcohol
• Caffeine (tea, coffee, cola, chocolate)
• Excessive dried fruit ( Prunes, figs, apricots etc.)
• Pure fruit juice
• Sorbitol (synthetic sweetener)
Trends with those injured longer
• Ageing – Getting older can affect function and ability, so bladder and bowel routines and management can also change.
• Dealing with incontinence – Always seek advice or help from your GP or spinal centre
• Incomplete emptying – Patients who tap and express occasionally have incomplete emptying and complain of sweating and having UTIs. They require a follow up to check that the bladder is functioning and fully emptying . Sometimes GPs diagnose this as a prostate problem in men, when it is actually a neurogenic bladder problem.
• Long term medication – Certain long term medication, such as Analgesia, can affect bladder and bowel function
• Bowel cancer screenings – These may be more difficult for spinal cord injured people, as the laxative administered as preparation for the colonoscopy may play havoc on your bowel routine. Be sure to talk to your GP before the procedure.
Useful links
https://www.waterfall-d-mannose.com/ – More information about Waterfall D-Mannose
http://www.bardmedical.co.uk/STATLOCKFoleyStabilisationDevice – StatLock catheter anchor
https://www.clinimed.co.uk/urology-continence-care/products/securement/clinifix – Clinifix catheter anchor
http://www.healthtalk.org/peoples-experiences/long-term-conditions/living-urinary-catheter/catheter-valves – Information about catheter valves
https://www.self.com/story/how-to-prevent-uti – UTI prevention guide
https://www.radarkeys.org/ – Information about radar keys
If you have questions about any of the issues raised in this article, please get in touch with our outreach team who may be able to refer you to organisations who can help. You can contact them via email or call them on 020 8875 1805.

